Key Points:
- Analysis looked at how oral anticoagulants might affect thrombectomy outcomes in stroke patients
- Outcomes similar whether patients on oral anticoagulants or IV tPA, or had normal hemostasis
Endovascular clot extraction is a safe and effective method of treating ischemic stroke among patients already receiving oral anticoagulation, according to a retrospective analysis published online October 15, 2015, ahead of print in Stroke.
“Although vitamin K antagonists (VKAs) and novel oral anticoagulants (NOACs) are the treatment of choice for stroke prevention, VKA with international normalized ratio (INR) > 1.7 and recent use of NOACs represent an absolute contraindication to intravenous tissue-type plasminogen activator (tPA),” Letícia C. Rebello, MD, of Emory University School of Medicine and Grady Memorial Hospital (Atlanta, GA), and colleagues write. Intra-arterial intervention may be an alternative to IV therapy, though data on “in the setting of anticoagulation are scarce,” they add.
Investigators led by Dr. Rebello reviewed prospectively-collected data on 604 consecutive patients receiving intra-arterial therapy, specifically thrombectomy, between October 2010 and March 2015. They compared outcomes of patients who received oral anticoagulation consisting of a VKA (n = 29) or NOAC (n = 17) with those having normal hemostasis (n = 265) or receiving IV tPA (n =297).
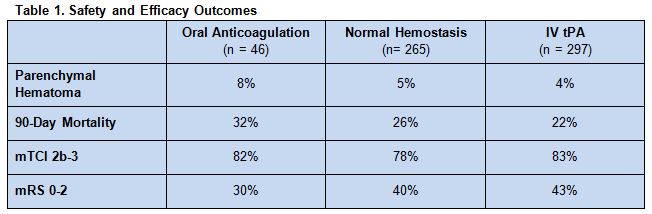
The primary safety endpoint was parenchymal hematoma, with 90-day mortality as a secondary safety endpoint. Efficacy endpoints were successful reperfusion, defined as a modified Thrombolysis in Cerebral Infarction rating (TCI) 2b-3 and good outcome, defined as a 90-day modified Rankin Scale (mRS) score of 0-2.
Baseline and outcomes variables were similar for patients who received VKAs and NOACS. Compared with those having normal hemostasis, however, patients who received oral anticoagulants were older (68.7 vs 64.0, P = .01), less likely to be active smokers (4% vs 19%; P = .01) and more frequently had A-fib (67% vs 24%; P < .01) and diabetes (41% vs 21%, P < .01). In addition, compared with patients on IV tPA, patients on oral anticoagulants had more A-fib (67% vs. 36%, P < .01), hypertension (86% vs. 70%, P = .02), and diabetes (41% vs. 24%, P =.02) and were less frequently active smokers (4% vs. 22%, P < .01).
Overall, there were no statistically significant differences in either safety or efficacy outcomes among the 3 patient groups (table 1)
Although cases of parenchymal hematoma trended higher with oral anticoagulants, multivariate logistic regression analysis confirmed that the drugs did not increase risk.
Endovascular Therapy the Best, Possibly the Only Option
“A-fib increases the risk of ischemic stroke up to 5-fold, and [oral anticoagulants are the treatment of choice for stroke prevention among this group of patients,” Dr. Rebello told WLNCMD in an email. “Moreover, A-fib accounts for as many as 25-40% of large vessel occlusion strokes, possibly leading to larger volumes, greater clinical severity, and a higher risk of hemorrhagic transformation. Due to its poor prognosis, it is extremely important to offer treatment to those patients.”
Unfortunately, IV tPA is contraindicated in patients receiving appropriate anticoagulation for A-fib. In a telephone interview with WLNCMD, Koto Ishida, MD, of NYU Langone Medical Center (New York NY), explained that treatment of ischemic stroke in patients taking novel anticoagulants is essentially limited to endovascular clot extraction. While research to date on this procedure for this indication has been positive, patient numbers have been small.
“Our study adds to the available literature supporting the safety of endovascular treatment in patients taking oral anticoagulants,” added Dr. Rebello. “Given the poor prognosis of stroke related to A-fib and the fact that therapeutic anticoagulant usage is a contraindication for IV tPA, we believe that endovascular treatment should be pursued.”
The only other treatment option, Dr. Ishida said, would be to use IV tPA off-label in these patients, but that is risky. “People hesitate, especially with this new generation of blood-thinning medicines that we are still learning about,” she commented. “The complications and outcomes when you have bleeding on these new medicines are unclear, and the antidotes being developed are not widely clinically available as of yet, so if you do have bleeding, it’s even harder to reverse.”
As NOACs are increasingly used, the number of patients taking these medications who require treatment for ischemic stroke will only increase, offering enough candidates to perform a randomized clinical trial. Both Dr. Rebello and Dr. Ishida acknowledge that is what is needed to conclusively determine the best course of action in this patient population.
Source:
Rebello LC, Haussen DC, Belagaje S, et al. Endovascular treatment for acute ischemic stroke in the setting of anticoagulation. Stroke. 2015;Epub ahead of print.
Disclosures:
- Drs. Rebello and Ishida report no relevant conflicts of interest.